





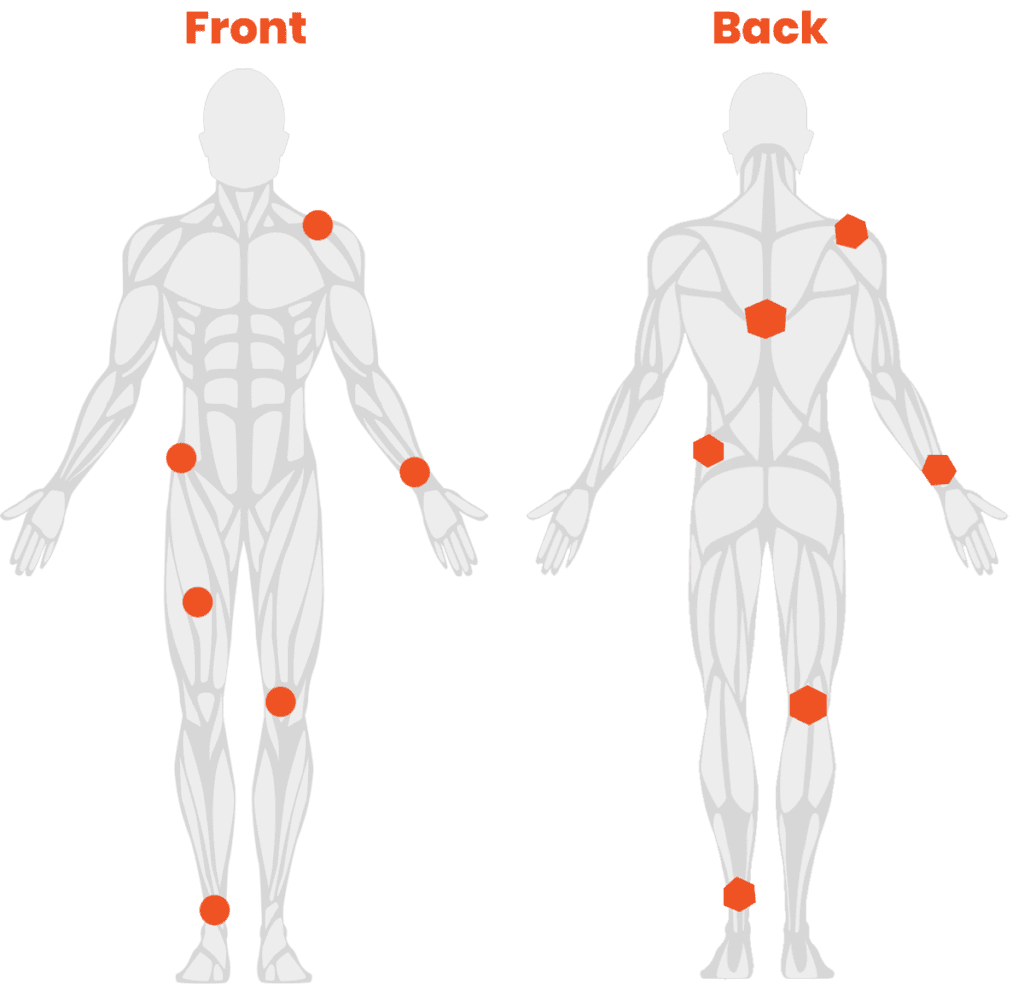
Shoulder
Shoulder pain is a common ailment that affects thousands of people in the US each year. In some cases, shoulder pain can be commonly mistaken for pain that is being referred from your neck.
Leg
Pain in the legs can have many different causes. From sharp shooting pain, typically referred to as sciatica, to a dull and achy heaviness, symptoms can vary greatly.
Knee
Knee pain is a common ailment that affects thousands of people in the US each year. There are several different structures in the knee, each of which can be damaged by several different causes.
Shoulder
Shoulder pain is a common ailment that affects thousands of people in the US each year. In some cases, shoulder pain can be commonly mistaken for pain that is being referred from your neck.
Knee
Knee pain is a common ailment that affects thousands of people in the US each year. There are several different structures in the knee, each of which can be damaged by several different causes.








Monday: 9:00 AM – 8:00 PM
Tuesday: 9:00 AM – 8:00 PM
Wednesday: 9:00 AM – 8:00 PM
Thursday: 9:00 AM – 8:00 PM
Friday: 9:00 AM- 6:00 PM
Sat-Sun: CLOSED
311 Spotswood Englishtown Road
Monroe Township, NJ 08831
732-641-4814
Monday: 9:00 AM – 8:00 PM
Tuesday: 9:00 AM – 8:00 PM
Wednesday: 9:00 AM – 8:00 PM
Thursday: 9:00 AM – 8:00 PM
Friday: 9:00 AM- 6:00 PM
Sat-Sun: CLOSED